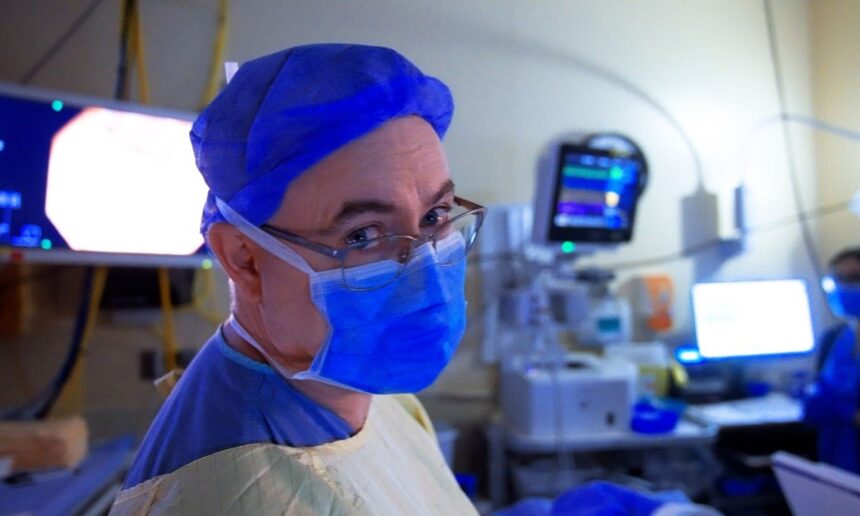
Last April, I sat in on a conversation with an endoscopy nurse at Langley Memorial Hospital. She described watching a small, pale polyp appear on the screen during a routine colonoscopy—one she might have missed a year earlier. This time, a blue box flickered around it. The AI had seen what her eye nearly didn’t.
That moment, small as it was, is now being replicated across twelve hospitals in the Fraser Health region. The GI Genius system, an artificial intelligence tool that highlights suspicious tissue during colonoscopies, has quietly expanded from a single pilot site to become part of standard care for thousands of patients across the Lower Mainland and Fraser Valley. It’s a shift that reflects both the promise of medical technology and the urgency of a disease that’s moving in the wrong direction among younger Canadians.
March is Colorectal Cancer Awareness Month, but the numbers don’t need a calendar to matter. Colorectal cancer remains the second leading cause of cancer death for men and the third for women in Canada, according to national data. What’s more unsettling is the trend among people under fifty. Colorectal Cancer Canada reports that the average forty-five-year-old today carries the same risk as a fifty-year-old did in 1979. The disease is appearing earlier, and the health system is scrambling to keep pace.
Dr. Scott Cowie, a surgeon at Langley Memorial Hospital who helped bring the technology to Fraser Health, describes the tool as a second set of eyes. During a colonoscopy, the AI scans video in real time, marking polyps—the small growths that can turn cancerous—with visual cues on the screen. The endoscopy team still makes every decision, but the algorithm offers a kind of vigilance that doesn’t blink or tire.
“We’re using this technology to support better detection, more consistent quality, and smarter decision-making during colonoscopy,” Cowie says. The language is measured, but the implication is clear. In a procedure where missing even one polyp can mean the difference between prevention and cancer, consistency matters as much as skill.
Fraser Health introduced GI Genius in 2023 at Langley Memorial as part of its colon cancer screening program. The expansion now includes Abbotsford Regional Hospital and Cancer Centre, Burnaby Hospital, Chilliwack General Hospital, Delta Hospital, Eagle Ridge Hospital, Peach Arch Hospital, Royal Columbian Hospital, Ridge Meadows Hospital, Surrey Memorial Hospital, Mission Memorial Hospital, and the Jim Pattison Outpatient Care and Surgical Centre. The rollout reflects both the system’s early success and the region’s capacity to integrate new tools without disrupting existing care pathways.
What makes the technology compelling isn’t just what it finds, but what it might eventually help clinicians leave alone. Fraser Health is now exploring a next-generation version of the software that could help physicians better characterize very small polyps during the procedure itself. Some of these growths are benign and pose no cancer risk. Removing them anyway adds cost, discomfort, and lab work that may not change outcomes.
“This is an encouraging development because it may help us avoid removing certain benign polyps that do not require excision, while still maintaining a strong focus on safety and quality,” Cowie adds. It’s a careful balance—err too far on caution and you overwhelm the pathology system with unnecessary biopsies; lean too hard on efficiency and you risk missing something that matters.
The stakes are high because the outcomes are so stark. When colorectal cancer is caught at its earliest stage, survival rates exceed ninety percent. That figure drops sharply as the disease progresses. Screening, then, is less about individual heroism and more about infrastructure—getting the right people tested at the right time with the right tools.
In British Columbia, average-risk residents aged fifty to seventy-four are eligible for fecal immunochemical testing, a non-invasive stool test that checks for hidden blood. Those with a family history, genetic markers, or other risk factors may be referred directly for colonoscopy. The symptoms worth watching for include blood in the stool, persistent abdominal pain, changes in bowel habits, and unexplained weight loss. They’re not subtle, but they’re often ignored or misattributed, especially in younger patients who don’t expect to be at risk.
The decline in colorectal cancer rates among older Canadians is a public health success story rooted in decades of screening advocacy and infrastructure investment. But the rising incidence among younger adults complicates that narrative. Researchers are still untangling why this is happening—diet, sedentary lifestyles, environmental exposures, and shifts in the gut microbiome are all under investigation. What’s clear is that the health system can’t wait for definitive answers before responding.
AI-assisted colonoscopy isn’t a cure, and it won’t replace the need for better prevention strategies or earlier screening guidelines. But it does offer something valuable in the meantime: a marginal improvement in detection that, multiplied across thousands of procedures, could translate into lives saved and cancers caught before they spread.
I think back to that nurse at Langley Memorial, and the blue box that appeared on her screen. It wasn’t magic. It was pattern recognition, trained on thousands of colonoscopy images and refined through clinical feedback. But in that moment, it was enough. And across twelve hospitals in the Fraser Valley, that enough is starting to add up.